Why Stretching Your Hips Isn’t Fixing Your Sciatica or Back Pain
You've Stretched. You've Rolled. You're Still Hurting.
Picture this: you wake up, your lower back is tight, and that familiar ache is already radiating into your glute or down your leg. So you do what makes sense — you pull your knee to your chest, hold a pigeon pose, run the foam roller along your IT band, and fire up the massage gun on your piriformis.
For about twenty minutes, you actually feel better.
Then you sit at your desk for an hour, stand up, and the tightness is right back where it started. The next morning, same thing. After enough cycles of this, it's easy to start wondering whether your body is just permanently wired this way — or whether you're missing something that no amount of stretching is going to fix.
Here's the truth: you're probably not doing anything wrong. But you may be pointed at the wrong target.
Stretching and foam rolling are fine tools. They're just often solving the wrong problem. Because mobility is rarely the missing piece for chronic sciatica and low back pain. What's actually missing is usually much harder to find on YouTube.
Why Stretching Temporarily Works — And Why That's a Problem
Stretching isn't useless. Let's be clear about that.
When you stretch a tight muscle, a few real things happen: circulation improves, neural tension eases slightly, and the nervous system — which is largely in charge of how much tension a muscle is holding — gets a brief signal to back off. That's real, and that's why it feels good.
The problem is why that tension came back in the first place.
Your body is not malfunctioning when your hips feel tight ten minutes after you stretched them. It's doing exactly what it's designed to do: creating tension where it perceives instability or threat. That tightness is, in many cases, a protective response — not a flexibility deficit.
If the underlying reason your nervous system is guarding hasn't changed, neither will the tightness. You can stretch your piriformis twice a day indefinitely. If the system doesn't trust the movement patterns supporting it, the piriformis will keep doing its job: getting tight.
This is one of the most frustrating cycles in musculoskeletal care, and it's one of the most common things we see during a first visit — especially among active adults in Brooklyn who are already putting in real effort to take care of themselves.
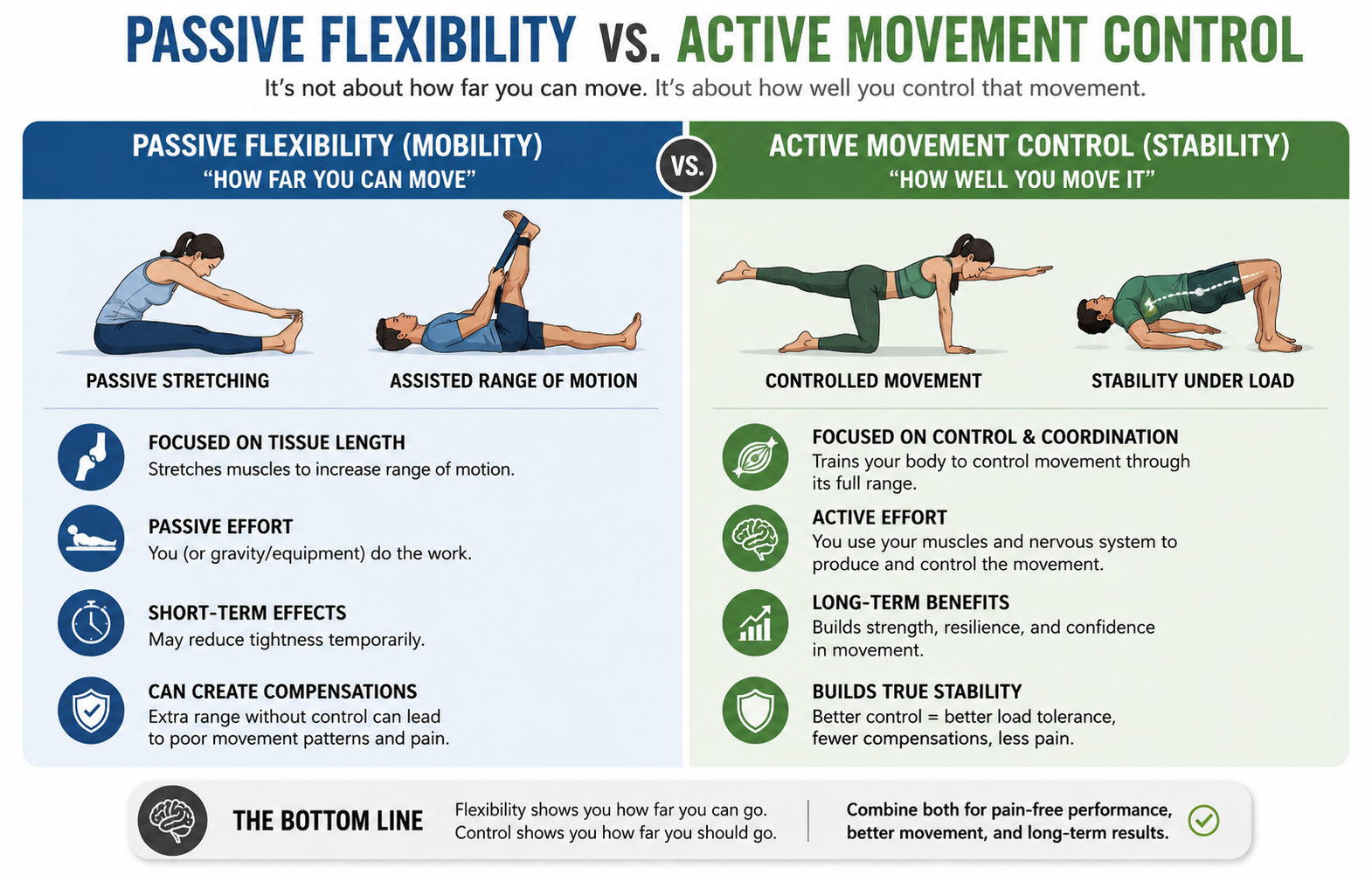
Mobility vs. Stability: What Most People Get Backwards
Here's a concept worth sitting with, because it changes the whole conversation.
Mobility is range of motion — how far a joint can move. Stability is the ability to control that movement through that range.
These are entirely separate things.
And people with persistent hip tightness and back pain often have plenty of the first and almost none of the second.
Think about a Brooklyn desk worker who sits eight or nine hours a day, then comes home and does twenty minutes of hip flexor stretching. Their hip flexors are probably not the problem. Their body has been parked in a shortened position so long that their glutes have essentially stopped contributing to how they move.
When they get up and start walking, something else has to pick up the slack — and that something else, usually the low back extensors or the piriformis, ends up doing double duty.
Or consider a gym-goer who squats and deadlifts regularly but still wakes up with chronic low back stiffness. They have the hip mobility to get into good positions. What they often lack is the spinal segmental control to maintain those positions under load. Every rep, the lumbar spine compensates. The muscles around it tighten to protect it.
Brooklyn pickleball players are another example we see regularly. The rotational and lateral demands of the game are high — and players dealing with recurring glute pain or sciatic symptoms often have perfectly adequate hip mobility. What's missing is the capacity to decelerate, stabilize, and absorb force through one leg when they're pushing off or changing direction hard.
Parents who spend years lifting kids off the floor are also in this boat. They're bending and rotating hundreds of times a day in patterns their bodies were never trained for. The hip range of motion is fine. The ability to control what the lumbar spine is doing during that movement isn't.
The common thread: mobility without stability and movement coordination often produces compensations, not solutions.
Why Sciatica and Back Pain Keep Cycling Back
Persistent Sciatica and low back pain are rarely explained by a single tight muscle or a single bad movement. They're usually the result of patterns — repeated loading strategies the body has been defaulting to for months or years.
Some of what drives the cycle:
Sensitized nerves. The sciatic nerve, like any tissue, can become irritated and sensitized over time. A sensitized nerve doesn't need a herniated disc pressing on it to fire — it can produce symptoms from relatively minor mechanical inputs like sustained sitting, hip flexion, or light compression. Stretching an irritated nerve is sometimes helpful and sometimes counterproductive, depending on the direction and the load.
Poor hip-spine coordination. The lumbar spine and the hip are supposed to share the work of bending, rotating, and absorbing load. When one of them stops pulling its weight, the other overworks. In most people with chronic back pain, the hips are undercontributing and the lower back is picking up the difference — on every single movement, hundreds of times a day.
Sitting and bending intolerance. Many people with back pain gradually lose tolerance for sustained postures: sitting for more than twenty minutes, bending to tie their shoes, loading the spine in flexion. These aren't catastrophic problems — but they do tell a specific story about what movements need to be retrained and in what order.
Deconditioning. Pain changes how people move. People with persistent back pain often stop loading their spine and hips through full ranges because it hurts — which makes sense in the short term. But reduced loading over time means reduced tissue capacity, which makes the whole system more vulnerable to the next provocation. Breaking that cycle requires progressive, graded loading — not avoidance.
None of this is meant to be alarming. These are mechanical, trainable problems. They just don't respond well to stretching alone.
Common Mistakes People Make With Sciatica and Hip Tightness
Most people dealing with these symptoms aren't doing anything reckless. They're following reasonable-sounding advice — they just haven't been given the full picture. Here are a few patterns worth reconsidering:
Aggressively stretching an already irritated nerve. When the sciatic nerve is sensitized, certain stretching positions — deep hip flexion, straight-leg toe touches, seated hamstring stretches — can actually load the nerve rather than release it. If your stretching routine reliably provokes symptoms that linger, that's the nerve telling you something.
Foam rolling the painful area constantly. Foam rolling can reduce muscle tension temporarily and improve circulation. But repeatedly compressing an area that's symptomatic isn't addressing why the tissue is unhappy — it's just managing the output. If you need to roll the same spot every morning to function, that's a signal worth following up on.
Avoiding all movement. Rest has a role when symptoms are severe. But extended movement avoidance leads to deconditioning, which makes the system more — not less — vulnerable. Most people with sciatica and back pain need better movement, not less of it.
Chasing temporary relief instead of root causes. Heat, massage, stretching, and passive care all have value. The issue is when they become the entire plan — a revolving door of short-term relief without any progress on the underlying drivers.
Copying social media mobility routines without context. Not all mobility work is interchangeable. A thoracic rotation drill that helps a healthy athlete might do nothing — or worse, irritate things further — for someone with active nerve symptoms. Individual presentation matters enormously.
What a Rehab-Based Approach Actually Looks Like
This is where the conversation shifts.
At Functional Rehab in Brooklyn, the starting point for every patient with Sciatica or Back Pain is a thorough movement assessment — not a quick adjustment and a paper exercise handout.
A good assessment identifies the specifics: which movements provoke symptoms, which movements relieve them, where the spine is losing control, which muscle groups aren't contributing, and how the hip and spine are coordinating (or not). That information drives everything that comes after.
From there, the approach is built in layers:
Improving spinal positioning. Before anything else can be trained effectively, the spine needs to be able to find and maintain positions that reduce mechanical stress. For many people with sciatica, a specific directional strategy — often extension-based — creates a significant symptom shift before any other intervention is needed.
Restoring hip control. Getting the glutes and deep hip stabilizers actually working again — not through generic activation exercises, but through movement patterns that are relevant to what the person actually does. Whether that's sitting at a desk all day, squatting in the gym, or pushing off hard on a pickleball court.
Manual therapy where it makes a meaningful difference. Hands-on work can reset tissue tension, improve joint mobility, and calm down irritated areas. But in a rehab-forward model, it's a catalyst — not a substitute for movement retraining.
Progressive loading. The end goal is a body that can handle more — not one that needs to permanently avoid what used to hurt. Progressive loading through appropriate ranges builds the tissue capacity the system was missing.
Improving movement tolerance. Sitting tolerance, bending tolerance, walking capacity, sport-specific demands. These get trained specifically, not hoped for.
This is what separates a Rehab Chiropractor’s rehab-focused approach from treatment models that rely primarily on passive care without movement retraining — where something is done to you each visit, but nothing about how you move actually changes.
Overview of the movement assessment process
3 Exercises That May Help More Than Endless Stretching
These aren't replacements for a proper evaluation — but for many people dealing with sciatica or chronic low back pain in Brooklyn, these movements address what stretching misses. Watch the demonstration videos before attempting them.
Press Ups
Press Ups load the lumbar spine into extension using the arms, keeping the hips and legs relaxed. For people whose sciatica or back pain tends to get worse with sitting and bending — and better with standing or walking — this direction of movement often provides meaningful relief. It's one of the foundational movements used early in directional preference rehabilitation.
Press Ups can help reduce stiffness and irritation in some cases of low back pain and sciatica — especially when symptoms worsen with sitting and bending.
Focus on relaxing the hips and legs while letting the arms gently extend the spine. Move slowly and stay within a comfortable range.
Book Openers
Book Openers work on thoracic (mid-back) rotation while keeping the hips relatively still. Because the thoracic and lumbar spine are supposed to share rotational load, a stiff mid-back forces the lumbar spine to overcompensate — especially in rotational activities like golf, pickleball, and overhead lifting. This exercise helps restore mobility where it belongs, taking stress off the lower back.
Book Openers help improve rotation through the thoracic spine (mid-back) while reducing unnecessary stress on the lower back.
Move slowly, keep the hips relatively still, and focus on creating rotation through the upper back rather than forcing the movement.
Braced Leg Lifts
Braced Leg Lifts train the ability to move the hip independently from the lumbar spine — one of the most important coordination skills for people with back pain. Many patients with persistent symptoms have never learned to dissociate hip movement from spinal movement. This exercise builds that pattern in a low-load, controlled way, and serves as a foundation for more demanding movements later.
Braced Leg Lifts help train the ability to move the hip independently from the lower back — an important coordination skill for reducing unnecessary spinal stress.
Focus on keeping the core gently braced and the spine quiet while the hip does the movement. Slow, controlled reps are more important than height or speed.
When It's Time to Stop Self-Treating
Self-directed exercise has real value. But some presentations need professional evaluation sooner rather than later.
Consider booking an appointment if you're experiencing:
Pain radiating below the knee, especially into the foot or calf
Numbness, tingling, or a pins-and-needles sensation in the leg or foot
Significant weakness in the leg, foot, or when standing on one leg
Symptoms that have persisted for more than 4–6 weeks without clear improvement
Pain that wakes you up at night or that's getting progressively worse despite rest
Bladder or bowel changes — these warrant urgent medical evaluation
Even without those red-flag symptoms, if you've been stretching and rolling consistently for weeks with no lasting improvement, that's a strong signal the current approach isn't reaching the root of the problem.
Contact / Book Appointment Page
Frequently Asked Questions
Why do my hips feel tight even when I stretch every day?
Persistent hip tightness after daily stretching is usually a sign that the body is creating protective tension rather than responding to a true flexibility deficit. The nervous system tightens muscles when it perceives instability or poor movement control — and no amount of stretching resolves that if the underlying coordination and stability issues haven't been addressed.
Can stretching make sciatica worse?
It can, yes. Certain stretching positions load the sciatic nerve directly — particularly deep hip flexion and straight-leg movements. If your stretching reliably provokes symptoms that persist afterward, the nerve may be sensitized and those positions may be adding irritation rather than reducing it.
What's the difference between mobility and stability?
Mobility is how far a joint can move. Stability is the ability to control movement through that range. Many people with chronic back pain and sciatica have adequate mobility — what they lack is the muscle coordination and spinal control to use that range safely and efficiently.
Why does my back pain keep coming back even after I feel better?
Recurring symptoms are usually a sign that the movement patterns driving the problem haven't changed. Temporary relief — from stretching, massage, or passive treatment — doesn't retrain how the spine and hips coordinate during everyday movement. Without addressing those patterns directly, the same mechanical stresses keep reproducing the same symptoms.
What does a rehab chiropractor in Brooklyn actually do differently?
A rehab-focused chiropractor starts with a movement assessment to identify the specific compensations and coordination deficits driving your symptoms — rather than treating a diagnosis generically. Treatment involves hands-on care combined with progressive movement retraining tailored to your daily demands, with the goal of improving what you can do, not just managing how you feel.
The Bottom Line
Stretching feels productive. It offers temporary relief and it's something you can do on your own, which genuinely matters. But for most people with recurring Sciatica or chronic back pain, the issue isn't that the hips aren't flexible enough — it's that the spine and hips aren't stable or coordinated enough to sustain whatever gains the stretching produces.
That's a different problem, and it requires a different kind of solution.
If you're in Brooklyn and you've been caught in the stretch-feel-better-then-tight-again cycle longer than you'd like, Functional Rehab offers a comprehensive movement-based evaluation designed to identify what's actually driving your symptoms — and build a specific plan to address it.
No generic protocols. No passive-only treatment. A clear picture of what's happening and a direct path toward getting back to what matters to you.
Book a movement assessment at Functional Rehab
Functional Rehab is located at 597 Degraw Street in Brooklyn's Gowanus neighborhood, right above CrossFit South Brooklyn. We specialize in movement-based chiropractic and rehabilitation for active adults dealing with back pain, sciatica, and performance-limiting injuries.